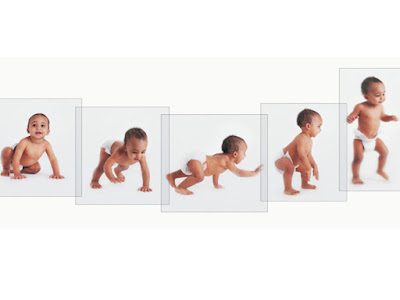
Red Flags: An Early Intervention Guide
by Trisha Roberts
Is my Baby delayed?
Does my Baby have a problem? These are questions parents frequently ask in
relation to their newborn, baby, or toddler.
This is an article compiling some of the “Red Flags” that indicate that
there MIGHT be a problem. “Red Flags”
are warning signs that there may be delays in development or something more
serious that warrants further investigation. Red Flags are a signal to parents
and care providers that they should initiate a discussion with their pediatrician. Multiple Red Flags are a strong indicator of
a potential problem and should signal parents and physicians to seek an
evaluation by an Early Intervention Therapist or Team of Evaluators specializing in child development.
General Red Flags
Signs of stress-
especially frequent or “interfering” changes in vitals (Heart Rate Fluctuations,
Baby seems to struggle to breathe, difficulty regulating temperature, etc.),
color changes, frequent yawning, finger splaying, excessive hiccups or gas
Poor head
control after 3 months
Arching of
back
Stiffening
of legs
Floppy or
limp body posture
Head
consistently turned or tilted to one side
Unusual
shape to head
Loss of
Language Skills at any age
Unequal
movements one side of the body compared to the other side of the body
Consistently
ignores one side of the body
Poor visual
tracking when head is supported
No leg
kicking when on back
No hand on
body exploration when on back
Poor sucking
at breast or bottle
Doesn’t
startle at loud sounds
Doesn’t turn
head to Mom’s voice
“Scissoring” or continual Crossing of legs
A child is displaying a Developmental Delay if there is a
failure to reach milestones appropriate for their age. Children develop at
their own rate, but there are normative charts for the average time frame for
major developmental achievements. If a
child is significantly outside of the normal range, it is considered a Red Flag.
The following are Red Flags by Age. NOTE:
If a Child was born prematurely, they will most likely be slower in
acquiring their developmental milestones of early childhood, but the
progression should follow the normal sequence, not necessarily the timing and
age range.
Red Flags By Age
 |
| Red Flags of Child Development by Age |
Red Flags 3 Months
Crosses eyes most of the time
Doesn’t seem to focus on Mom’s
face
Baby doesn’t “track” a toy (follow
a toy with his eyes from mid-line to right and left)
Doesn’t hold a toy if placed in
their hand
Doesn’t smile at father or mother
Red Flags 6 Months
One or both eyes turn out all the
time
Baby doesn’t reach for a grasp a
toy when held out front
Reaches with only one side
Does not bring toys or hands to
mouth
No rolling
Only using one arm
Poor midline orientation of head and
hands
No attempt to pull self to sitting
when hands are held
Cannot prop sit and falls over and
can’t catch themselves
Only gets out of sitting throwing body
backward
Does not bear weight through legs when
supported in standing
Seems to drag one side when crawling
on belly or on hands and knees
Shows no enjoyment in being around
people: doesn’t squeal or laugh, doesn’t like to cuddle, has no interest in
games like “Peek-a-Boo”, etc.
Does not move out of prone when placed
there
No Babbling
Doesn’t respond to their name
Cannot get in or out of sitting
position
Does not have some form of locomotion-
scooting, belly crawl, creeping
Multiple Ear Infections
Baby isn’t reaching, pointing, or
waving
Doesn’t point to objects or pictures
Doesn’t look for an object that is
dropped or covered up
Only uses one hand for grasping and
playing
Doesn’t take food off a spoon
Unable to pass a toy or object from
one hand to the other
Unable to stand briefly, if placed
Does not have a single word that
they use consistently (mama, dada, no)
Not pulling to standing
Not Cruising
Consistently walks on toes
Not picking up and eating finger
foods
Not Walking
Unable to get to standing from the
middle of the floor
If child has been walking for at
least 6 months, should be able to squat and return to standing
Only plays with one toy
Unable to squat to stand
Does not have stair mobility
No running
Doesn’t scribble
Trouble with
“playground skills:” unable to climb a ladder, seat self and slide; unable to
step over playground boundaries,
Falls on uneven surfaces consistently
Unsteady gait
Unable to jump down from a stable
object
Doesn’t follow simple instructions
Doesn’t point to body parts (“Where is
your nose?” “Where is your belly button?”)
Isn’t using 2-word combinations
Doesn’t imitate simple actions or
gestures
Doesn’t know the function of
common objects like a comb or glass (“What is this used for?”)
Unable to take off socks or hat
Unable to get on/off Riding toy
Unable to produce movement on a
Riding Toy
Unable to jump in place or jump
forward
Unable to build a tower of 6 or
more blocks
Doesn’t or try to imitate drawing
a circle or horizontal line
Eats with a spoon and very little
spilling
Unable to undress independently
Is not talking in sentences and
can’t be easily understood by strangers
Isn’t able to tell a simple story
Unable to gallop
Unable to skip
Fearful of playground equipment
Unable to hold a crayon correctly
Can’t draw a circle or square
What Should I do if my child is displaying Red Flags of Development?
Early intervention in the form of
Physical Therapy, Speech and Language Therapy and
Occupational Therapy can
dramatically improve a child’s development.
The sooner treatment starts, the better the prognosis and outcome--The “Let’s
Wait and See” is not the best approach. If a parent is concerned and has noted
several Red Flags, they should seek an evaluation of their child by a physician
or Early Intervention Therapist.
Therapy with an infant, baby or young child can significantly improve that child's overall function and development. Early Intervention Therapists will use
unique toys and activities that will engage your child in play and promote development. Your therapist will give you exercises, activities, and suggestions to help you help your child at home, at school, and in the community.
Regardless of the cause or severity of a problem, our Goal as Early Intervention Therapists is to maximize the potential of each child!
The Website associated with this Blog,
Proeducationaltoys.com has a wealth of excellent toys that can be helpful in advancing the skills of your child whatever their age or problem.
Click Here to visit
Proeducationaltoys.com
 |
| Toys are Used in Therapy to Promote Skills |
 |
| Children Learn Through Play |

|
| Therapists will Give Suggestions for Unique Toys and Activities to Help Advance Your Child's Development! |
Author: Trisha Roberts
www.proeducationaltoys.com
Copyright © 2016 TNT Inspired Enterprise, LLC,
All rights reserved.
Unauthorized duplication is a violation of
applicable laws.